Dermatology
Veins Vienna

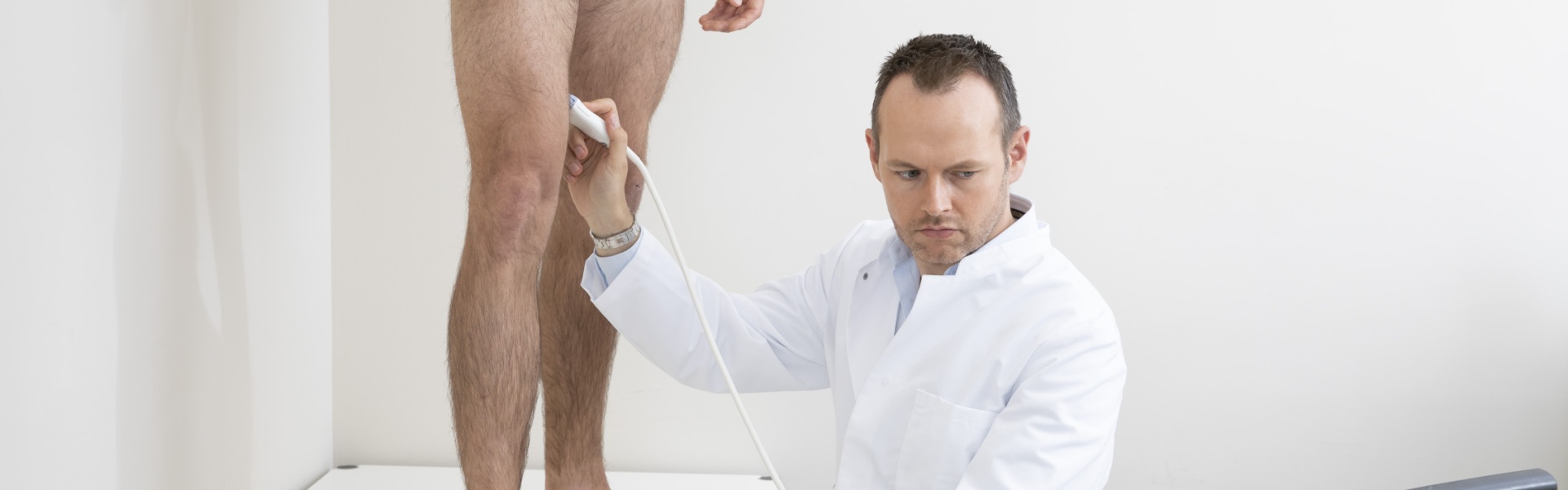
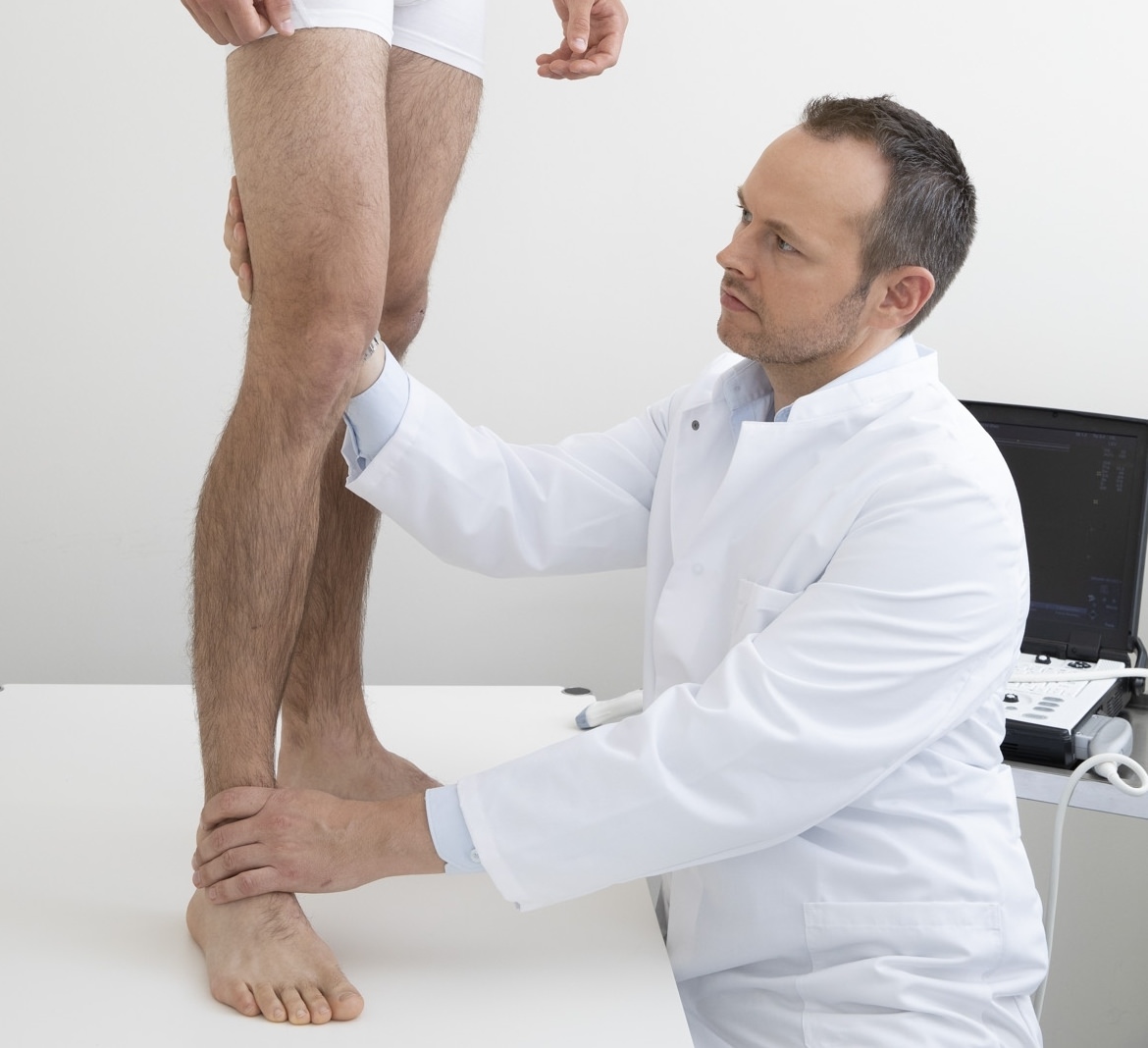
Vein function status using color-coded duplex sonography
Every vein treatment should start with proper diagnosis. Using modern, painless ultrasound technology, the venous vascular system of the leg is examined prior to any vein or spider vein treatment to identify any potential underlying problem.
Often spider veins and superficial varicose veins are a sign of venous valve incompetence of the truncal veins. Unless this is corrected, superficial therapy of visible veins and spider veins is not effective, as no lasting results can be expected. Long-term success can only be garnered through targeted therapy of the underlying problem.

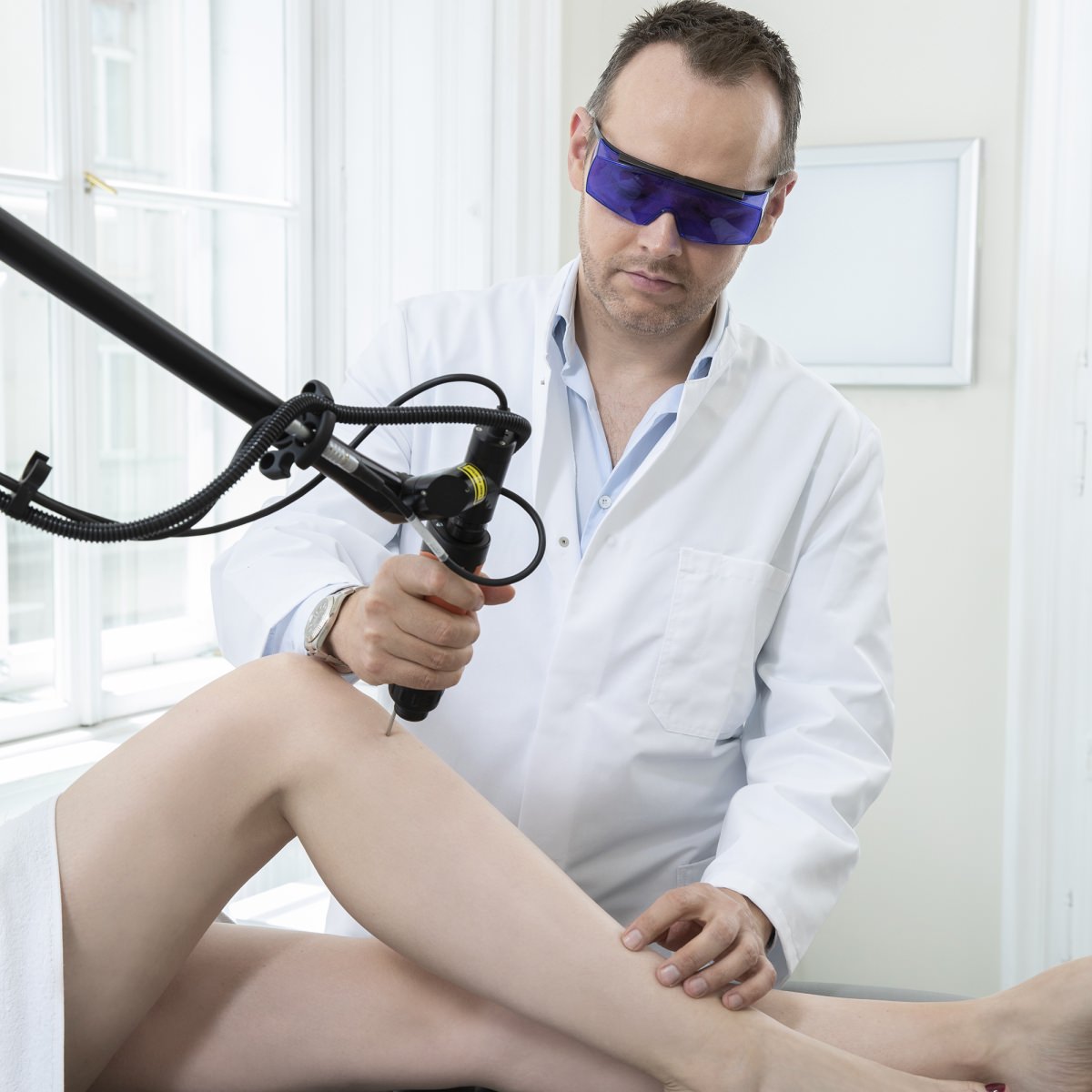
Sclerotherapy and laser therapy:
Beautiful legs through painless sclerotherapy of veins and spider veins
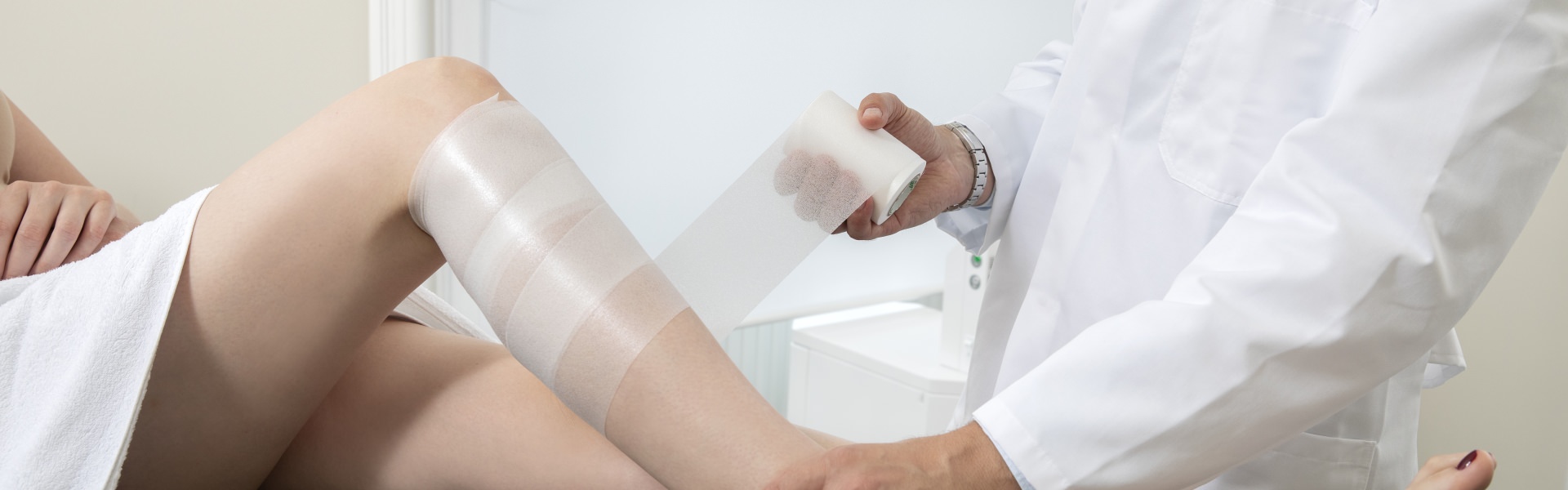
The sclerotherapy of spider veins and larger veins with sclerosing agents has established itself over decades as an integral part of the therapy of venous diseases. In most cases, sclerosing liquids or foam is injected into the affected vessels in several sessions.
After the treatment, a compression stocking should be worn for some time to achieve an optimal result.
Possible side effects are discoloration of the skin, bruising and rarely inflammation of the treated veins. These side effects are usually temporary and can usually be treated very effectively.

Minimally invasive vein surgery with radiofrequency ablation of veins
For patients with extensive incompetence of the superficial truncal veins, a surgical procedure is the best option. Here, the insufficient vein is punctured and closed from the inside by laser or radiofrequency, acrylate glue or other treatment modalities.
Endoluminal thermal ablation (closing of the vein with heat) has been shown to be equivalent to the classic stripping surgery of veins in several studies and is recommended as a first-choice method in several guidelines.
Dr Holzer offers endoluminal thermal ablation of varicose veins (closing of the vein with heat) using the Closure Fast® radiofrequency method, which has been a mainstay for varicose vein treatment for decades.
This operation is performed under local anaesthesia (tumescence anaesthesia). If desired, this procedure can also be performed under sedation. This operation is often supplemented by other procedures such as an ambulatory phlebotomy or sclerotherapy of smaller varicose veins.
Common side effects of the treatment include pain from needle punctures (only with local anaesthesia) as well as bruising and redness after the operation. Postoperative pain is extremely rare, as is thrombosis of the deep veins caused by the operation. This risk can be significantly reduced by anticoagulants, ample fluid intake and sufficient walking after the operation. A compression stocking should be worn for about 4 weeks after the procedure.


Ambulatory phlebotomy
Removal of superficial varicose veins
Visible varicose veins on the lower leg and thigh are removed via small incisions. The small incisions heal without scarring. Postoperative bruising and redness may occur, but these will heal on their own. Rarely, local temporary numbness may occur due to injury to skin nerves. This generally gradually wears off within 3 months. Wearing a compression stocking after the operation is also highly recommended in order to counteract these side effects.

In a proportion of patients, the regular wearing of compression stockings and the intake or local application of venous-active drugs can provide some relief from typical venous complaints such as swelling and heavy legs
However, not every patient is willing and able to put on the tight compression stockings and wear them during the day. Here, too, the individual needs and desires of the patient have to be taken into account.

Leg ulcers ("Ulcus cruris")
Leg ulcers are often caused by underlying pathologies such as venous reflux, which must be diagnosed and treated in order to achieve healing of the ulcer. In combination with consistent, regular wound therapy and additional surgical interventions, such as mechanical wound debridement and split-skin thickness wound grafts, it is possible to heal venous ulcers.